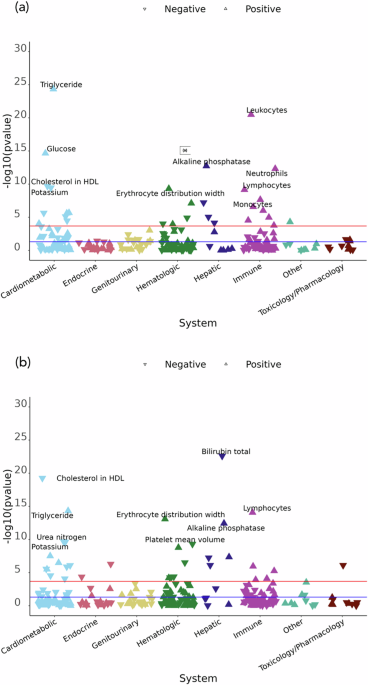
A major new study has identified a suite of blood-based biomarkers connected to posttraumatic stress disorder, offering a potential new path for objective assessment of the condition. By analyzing genetic and health record data from nearly 24,000 individuals, researchers pinpointed specific changes in liver, metabolic, and blood cell markers associated with a person's genetic liability to PTSD.
The research, conducted within a large health system biobank, used a two-pronged approach. First, it examined individuals' polygenic risk scores (PRS) for PTSD, which estimate genetic predisposition. Second, it identified patients with a clinical PTSD diagnosis in their electronic health records. Both groups were then analyzed for associations with 241 common laboratory tests. The triangulation method revealed 16 unique laboratory traits across cardiometabolic, hematologic, hepatic, and immune systems that were implicated by both genetic risk and actual diagnosis.
Further analysis using Mendelian randomization, a technique to infer causality, suggested that the genetic liability for PTSD may directly influence several of these biomarkers. The study found evidence of potential causal effects leading to decreased albumin and total bilirubin (liver function), decreased HDL cholesterol and increased VLDL cholesterol (cardiometabolic health), and decreased mean platelet volume (hematologic function). These findings move beyond correlation, indicating that PTSD risk may actively contribute to measurable physiological changes.
For patients, this work represents a hopeful step toward more concrete, biology-based tools for PTSD. The identified biomarkers are all derived from routine, scalable blood tests already used in clinical settings, meaning they could be more easily integrated into future diagnostic or monitoring protocols. This could help address the current reliance on subjective symptom reporting and improve the precision of treatment approaches.
Researchers emphasize that further validation in more diverse populations is essential before any clinical application. However, the study successfully demonstrates a powerful method for discovering clinically actionable biomarkers. The next phases of research will focus on replicating these findings and determining if tracking these biomarkers can help guide treatment decisions or predict patient outcomes, ultimately aiming to provide a clearer biological window into the complex experience of PTSD.