For years, the devastating impact of chronic traumatic encephalopathy, or CTE, has remained a shadow only visible after it is too late. This neurodegenerative condition, strongly linked to repeated head impacts in contact sports like football, has historically been confirmed solely through postmortem examination of brain tissue. This stark reality has left living patients and their families navigating a difficult journey of symptoms without a definitive answer. Now, however, a promising shift is on the horizon as dedicated researchers focus their efforts on bringing this diagnosis into the light of day, aiming to offer clarity and hope during a patient's lifetime.
At the forefront of this scientific pursuit are Drs. Chad Yucus and Julian Bailes, whose collaborative work represents a significant stride toward a future where CTE can be identified in the living. Dr. Bailes, a noted neurosurgeon and researcher, emphasizes the critical importance of this mission. The inability to diagnose CTE while a patient is alive has long been a major obstacle, not only for individuals and families seeking understanding but also for the development of targeted treatments and management strategies. Their research is dedicated to removing that barrier, transforming how the medical community approaches this complex condition.
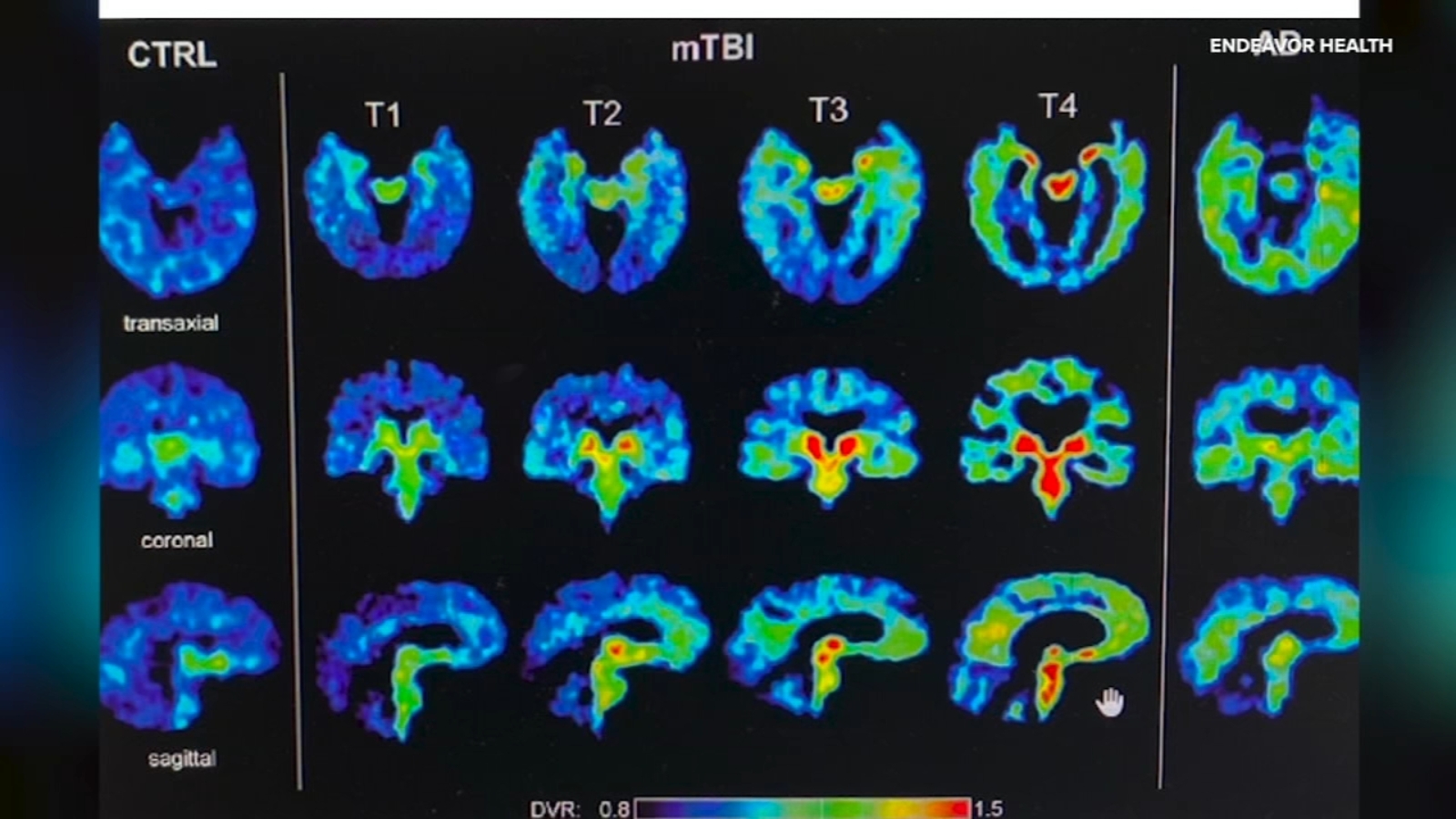
The core of their investigative work involves identifying specific biological markers, or biomarkers, that could reliably signal the presence of CTE. This process involves meticulous analysis and advanced imaging techniques to detect the unique signature of the disease within a living brain. While the path to a validated clinical test is rigorous and requires further study, each step forward builds a more robust foundation for future breakthroughs. The potential success of this research would mark a paradigm shift, moving the fight against CTE from a retrospective analysis to a proactive clinical framework.
Ultimately, the goal extends far beyond a simple diagnostic tool. A reliable method for identifying CTE in living patients would open the door to unprecedented possibilities for care and intervention. It would allow healthcare providers to better tailor support for symptoms, connect patients with appropriate resources, and, most importantly, accelerate the development of therapies aimed at slowing or stopping disease progression. For athletes, veterans, and others affected by head trauma, this work carries the profound hope of a day when a diagnosis comes with a roadmap for management rather than a postscript. The dedicated efforts of researchers like Yucus and Bailes are steadily illuminating a path toward that brighter, more hopeful future.