Clinical trials at a leading academic medical center are advancing new immunotherapies and testing platforms that could improve outcomes for patients with glioblastoma, an aggressive and difficult-to-treat brain tumor. These developments offer hope for a disease where the standard treatment has remained unchanged for nearly two decades and long-term survival remains low.
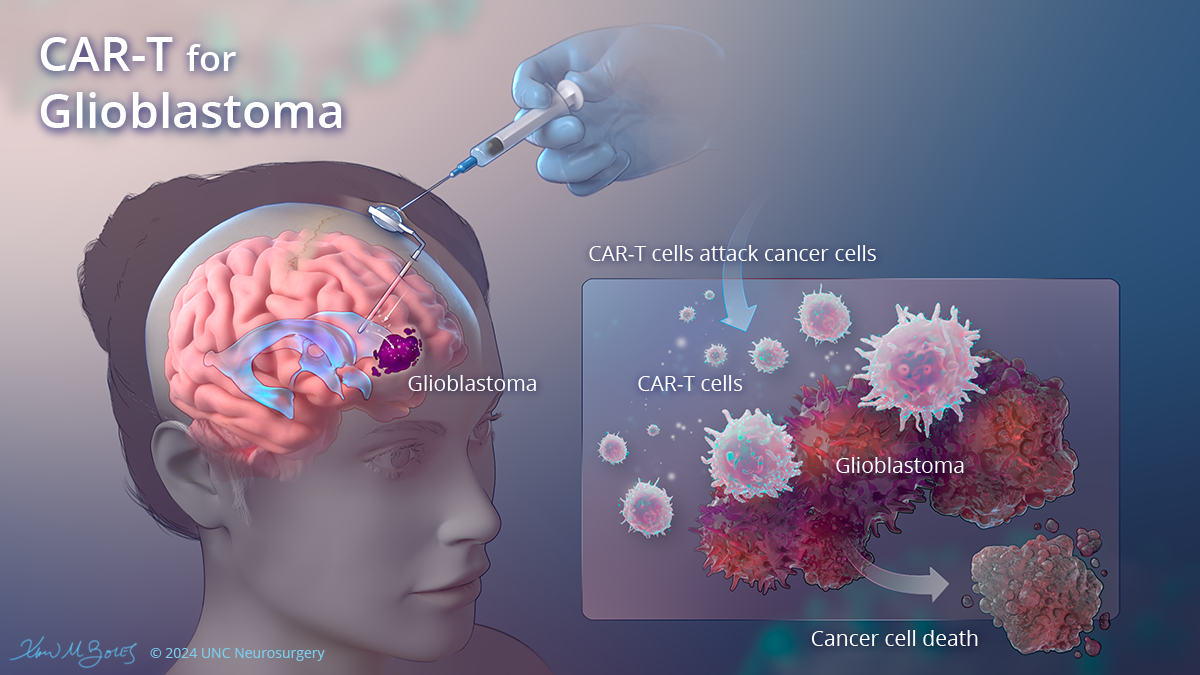
One approach involves chimeric antigen receptor T-cell (CAR-T) therapy, a treatment already used for some blood cancers. In an ongoing trial, a patient's own immune cells are extracted, genetically engineered to recognize a specific target on brain tumor cells, and then reinfused. These reprogrammed "hunter" cells are designed to seek out and destroy the cancerous cells. The trial is evaluating the safety and tolerability of this approach for patients whose glioblastoma has recurred after initial treatment.
Separately, a multicenter trial is assessing a novel immunotherapy called IGV-001. Following tumor-removal surgery, small biodiffusion chambers containing either the treatment or a placebo are implanted. IGV-001 is designed to stimulate a broad and durable immune response against the tumor. After six weeks, patients then begin the standard regimen of chemotherapy and radiotherapy. The trial aims to enroll 93 newly diagnosed patients to determine the treatment's safety and effectiveness.
Personalized Testing and New Research Pathways
Beyond new drugs, researchers are developing tools for more personalized treatment. Scientists have created a "brain slice" platform that keeps a patient's tumor tissue alive outside the body. This allows doctors to test various drugs directly on the sample to identify which therapy might be most effective for that individual's cancer before administering it to the patient, potentially saving crucial time.
Further research is focusing on specific receptors on glioblastoma cells, such as the epidermal growth factor receptor, which is crucial for cancer growth. Teams are using noninvasive imaging to track how these receptors change and how well therapies target them. This work complements surgical studies and aims to create a more detailed understanding of how to attack each tumor's unique biology.
The collective progress across these distinct fronts—from engineered cell therapies and novel immunotherapies to personalized testing tools—represents a significant and multifaceted research effort. While these are ongoing clinical studies and not yet approved treatments, they mark a hopeful shift toward more personalized and potent strategies for a cancer that urgently requires new options.